
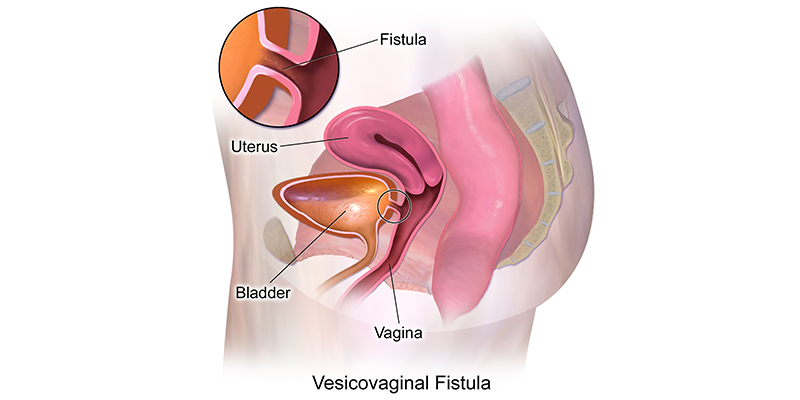
Vesicovaginal fistulae are usually secondary to obstetrical trauma, pelvic surgery, advanced pelvic cancer, or radiation therapy for treatment of pelvic cancer.
The basic principles for treatment of vesicovaginal fistulae have changed little since the mid-19th century work of Marion Sims. The principles are to ensure that there is no cellulitis, edema, or infection at the fistula site prior to closing the fistula and to excise avascular scar tissue and approximate the various layers of tissue broadside to broadside without tension. A 20th century addition to these principles is that of using transplanted blood supply from the vestibular fat pad, bulbocavernosus muscle, gracilis muscle, or the omentum.
The type of suture used appears less significant when the above principles are followed. In general, we have used the glycolic acid sutures such as Dexon or Vicryl because of their reabsorption and reduced tissue reaction. Many surgeons prefer, however, to use a non-absorbable monofilament suture of nylon or Prolene on the vaginal mucosa. These sutures should not be placed into the bladder mucosa. If they are left in the bladder for long periods of time, urinary stone formation will occur.
The purpose of the operation is to close the vesicovaginal fistula perman